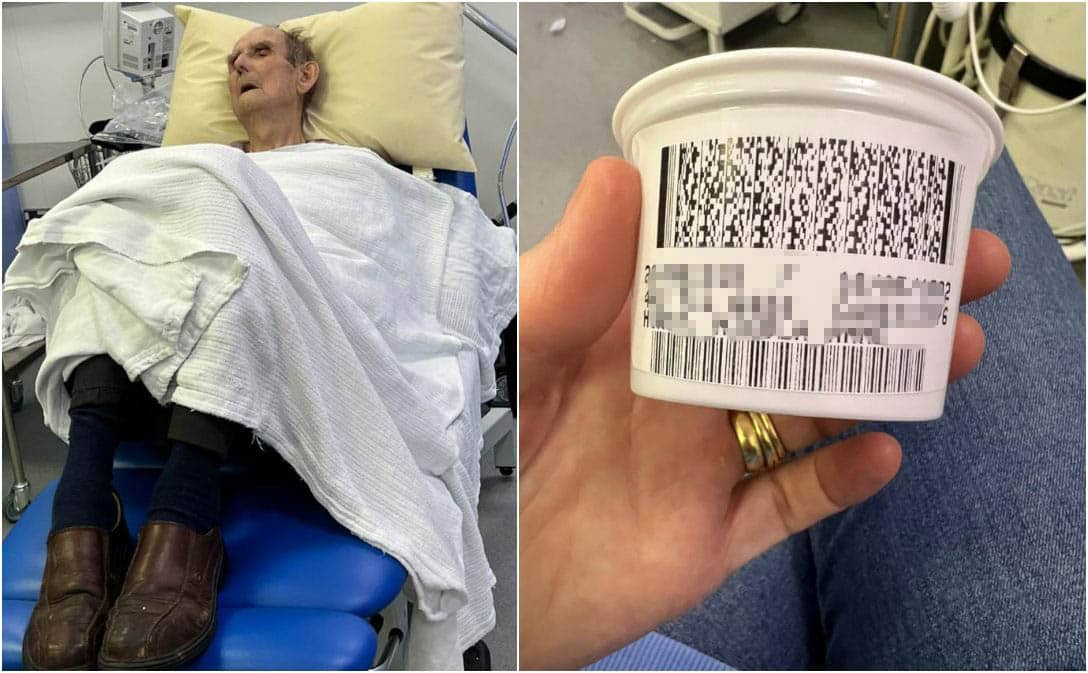
A frail 83-year-old man who spent 15 hours vomiting in a car outside Craigavon Area Hospital’s Emergency Department because there were no beds inside told his daughter he “would just be safer going and dying at home”.
Samuel Bailey was referred to the Emergency Department by his GP in Loughbrickland on Wednesday evening, suffering from suspected infections, including one of the lung.
Samuel’s daughter, Rachel Russell, took him to Craigavon just before 6pm that day, however, it was 9.20pm – almost three and a half hours after first presenting at the Emergency Department – that he was even brought in for triage.
Shockingly, it would be another 15 hours before Samuel, who spent the night vomiting profusely in his daughter’s car, would see a doctor.
Speaking to Armagh I, 27 hours after first travelling with her dad to the hospital, an exhausted Mrs Russell – who had just arrived back home – said the whole experience was “just horrendous”.
While the wait was bad enough, Samuel’s experience inside the hospital was not much better.
“Dad was sitting out in the A&E for two and a half hours before he went into triage, sat being sick into a kidney dish,” Rachel explained.
“My daddy is so private, he would just hate anyone seeing him being sick but there he was having to be sick in this, the place packed, and not one person came to say, ‘we’ll bring him through, or get him on to a trolley just to lie down’. He was that weak he just wanted to lie down.”
In the end, Rachel felt she had no option but take her dad out of the hospital and into her car where he could at least lie back.
“I told the staff we were going to wait in the car; told them they had my number, to phone us. He was being violently sick the whole time. I don’t know how many kidney dishes I went back in for and every time I did I tried to speak to someone. I said, ‘look where abouts is my dad in the list?’, but it was getting changed all the time.
“He lay out in the car for 15 hours. Now they’re saying he could have pneumonia. Not that the car was cold, because it wasn’t, but it was just really uncomfortable for a man of 83-years-of-age. I don’t know what sort of NHS this is. It just goes beyond words.”
Those 15 hours were some of the worst of Samuel’s life and heartbreaking for his daughter Rachel who also felt helpless.
“He just kept saying ‘I’m on my way out, I’m on my way out’, and then he got a bit cross. Then he said ‘I would just be safer going and dying at home because there’s no point lying here in a car, waiting to be seen’.
“I was heartbroken for him and I’m cross because of the way things are. At the same time, I can understand that everybody’s being pushed but whenever you’re looking at your own dad, and you’re seeing the fear in his eyes, because he doesn’t know whether this is the end, or what’s happening to him, it’s truly heartbreaking.”
However, when Samuel eventually got to see a doctor – in the middle of Thursday morning – he was taken to what Rachel described as a room “where they put all the broken stuff, broken equipment, into”.
“When you hear about how bad things are, you think, there’s no way it can be that bad, but see when they put my dad down into that room where they do the plaster casts for people? Even the nurse, God love her, she came in and she says, ‘I can’t believe they’ve put you here’.”
Even more galling was the sample pot handed to Samuel with a random woman’s name on it. The questions that alone posed for Rachel and her father.
Said Rachel: “I gave it to the nurses and said ‘the doctor gave me this’. She turns round and she goes, ‘oh, this doesn’t surprise me’.
“I have to say the nurses were lovely. Like, they couldn’t have apologised any more than they did. They couldn’t believe that dad had waited 15 hours; they were a wee bit shocked at that, because you can imagine there were a few different shifts had happened in between. They couldn’t understand why they had waited that length of time.”
Rachel says what she is struggling to understand is why it took so long when there was a letter from her GP outlining the pressing issue.
“To me, there is an administration problem,” she said. “I had the letter that my dad’s doctor in Loughbrickland had given to say that he had this lung infection, that he needed antibiotics, but because he was vomiting, he couldn’t get the antibiotics in him.”
Rachel claims despite the letter from her GP, she was told to wait to go to triage and hold out for a doctor to become available.
“To wait three hours to see triage, it seems to be a bit long. For an 83-year-old man to go through all that from Wednesday tea-time until he got a proper bed on Thursday afternoon, was horrendous.
“And then to tell me that they thought that it could be a mini heart attack. I can’t understand why they can’t just look at what the doctor has written; he’s already been seen by his GP; that’s my problem that I can’t figure out why they don’t do this.”
The biggest shock for Rachel was the fact her dad was allowed to lie out in a car for 15 hours.
“I could see into it if he wasn’t being sick but he was being sick. And then when they brought us down to this so-called room, I just blew my lid – this was just not on. The nurses even said they couldn’t believe that he was even taken down there. It was unreal.
“The nurses were very, very nice but you would nearly think that they’re asking for help themselves, for someone to speak up for them nearly, because they’re just at their wits’ end.”
Have you, or someone close to you, had a similar experience. Get in touch with Armagh I here – or comment below.
A spokesperson for the Southern Health Trust told Armagh I: “We very much regret the excessive waiting times being experienced by our patients and the impact this is having on our patients. Like other hospitals across Northern Ireland, our hospitals continue to work far beyond the capacity that is available and many patients are waiting a very long time in Emergency Departments to be admitted to a hospital ward.
“We are facing ongoing challenges in admitting patients and managing these pressures is a huge ongoing daily challenge for our exhausted staff. Most of the long waits in the Emergency Department are due to patients waiting for a bed to become available following another patient’s discharge. This has a direct impact on the length of time new patients who arrive at the Department will have to wait to be seen. It is vital that patients leave the hospital immediately when medically fit for discharge by accepting the first placement that becomes available including in the patient’s own home.
“Our hard-working staff continue to provide care and treatment to patients with emergency medical conditions attending our Emergency Departments. Staff are doing everything they can to make patients comfortable and treat everyone as safely and quickly as possible.
“Whilst we are unable to comment on an individual patient, we take all concerns about the care we provide extremely seriously and we encourage any patient/family member with concerns about our services to contacting our Service User Feedback team. Each concern/complaint is fully investigated before we send a comprehensive response back to the person making the complaint. The team can be contacted by telephoning (028) 37564600 or by emailing serviceuserfeedback@southerntrust.hscni.net.
“The Covid-19 global pandemic is still ongoing in our local community. The number of Covid-19 cases in our hospitals has been increasing recently. We urge patients to help keep themselves and others safe by: wearing a mask, washing hands, getting vaccinated, staying apart and leaving the hospital immediately when medically fit for discharge. Please remember to Phone First if you are thinking of coming before 9pm to our Emergency Departments with urgent but not life threatening symptoms – Tel: 0300 123 3 11. It is absolutely vital that people only attend our Emergency Departments if they require emergency treatment and consider using other options (GP, local pharmacies, MIU, GP Out of Hours etc..) where appropriate.”




